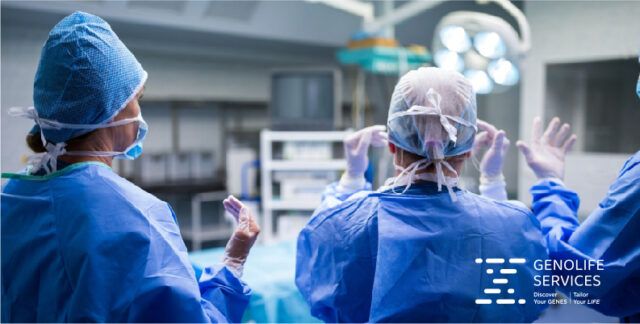
Many surgical procedures require General Anesthesia to induce unconsciousness and provide analgesia. This process is strictly monitored by Anesthesiologists and anesthesia care teams.
While modern anesthesia is exceptionally safe, some individuals carry a genetic predisposition that causes a life-threatening reaction to specific anesthetic agents. This condition is known as Malignant Hyperthermia (MH) (1).
Fortunately, proactive genetic screening now allows for pre-operative risk assessment, enabling clinicians to implement personalized, “safety-first” anesthesia plans.
What is Malignant Hyperthermia (MH)?
Malignant Hyperthermia (MH) is a hypermetabolic crisis triggered by volatile inhalational anesthetics and the depolarizing muscle relaxant Succinylcholine. These agents trigger an uncontrolled release of calcium from the sarcoplasmic reticulum into the skeletal muscle cells (1,2), leading to accelerated metabolism and a rapid rise in body temperature.
Key Clinical Manifestations during surgery include:
-
Fulminant Hyperthermia: Core temperature may escalate to 40–43°C.
-
Tachycardia and Tachypnea: Rapid heart rate and breathing.
-
Muscle Rigidity: Specifically masseter muscle rigidity or generalized stiffness.
-
Metabolic Derangements: Rhabdomyolysis, metabolic acidosis, and hyperkalemia.
-
Cardiac Arrhythmias.
Triggering Agents (per CPIC/PharmGKB guidelines) (2):
All volatile inhalational agents (e.g., Sevoflurane, Desflurane, Isoflurane, Halothane) and Succinylcholine.
Note: Intravenous agents such as Propofol and Ketamine are non-triggering and considered safe for MH-susceptible patients.
Epidemiology and Mortality Rates
MH is a rare phenomenon, with an incidence ranging from 1 in 5,000 to 1 in 100,000 anesthetic administrations (3). Despite its rarity, its onset is acute and potentially fatal.
The Impact of Early Diagnosis and Dantrolene:
-
Pre-Dantrolene Era: Mortality rates exceeded 80%.
-
Current Era (Early Diagnosis + Dantrolene): Mortality has fallen to <5–10%.
The critical factor in survival is prior knowledge of susceptibility.
Sources: Rosenberg H et al. GeneReviews® (1) | Cong Z et al. Clin Genet. 2024 (3)
The Genetic Basis of MH
MH is a pharmacogenetic disorder linked to mutations in genes regulating calcium homeostasis in skeletal muscles (1,2). Key genes identified by ACMG Secondary Findings v3.2 (2023) (5) and CPIC/PharmGKB (2) include:
-
RYR1: The primary gene encoding the ryanodine receptor; mutations are found in 50–70% of MH cases.
-
CACNA1S: Encodes a subunit of the voltage-gated calcium channel (~1% of cases).
-
STAC3: Associated with specific myopathies and increased MH risk.
Inheritance Pattern: MH follows an Autosomal Dominant pattern.
-
If a parent carries a pathogenic variant, each child has a 50% chance of inheriting the risk.
-
First-degree relatives of a known MH-susceptible individual should undergo formal risk assessment.
-
Individuals carrying the mutation may remain asymptomatic until exposed to a triggering anesthetic agent.
Diagnostic Modalities
-
Genetic Testing: A non-invasive blood test to identify pathogenic variants in RYR1, CACNA1S, or STAC3. Identifying a known mutation confirms Malignant Hyperthermia Susceptibility (MHS).
-
IVCT / CHCT (In Vitro Contracture Test): The Gold Standard for diagnosis (2,6). It involves a muscle biopsy to observe the muscle’s contractile response to caffeine and halothane. This is typically performed at specialized centers and is reserved for cases where genetic results are inconclusive or family history is highly suggestive.
Clinical Indications for Screening
Per CPIC/PharmGKB (2) guidelines, screening is recommended for individuals with:
-
A personal history of adverse reactions during anesthesia (rigidity, unexplained fever).
-
A confirmed family history of MH.
-
Underlying myopathies (e.g., Central Core Disease or Multiminicore Disease).
-
A history of unexplained exertional rhabdomyolysis or heatstroke.
-
Patients scheduled for surgery involving inhalational anesthesia who have familial risk factors.
Enhancing Surgical Safety through Precision Medicine
Identifying MHS prior to surgery allows the surgical team to:
-
Utilize Total Intravenous Anesthesia (TIVA) using Propofol or Ketamine.
-
Ensure the immediate availability of Dantrolene in the operating suite.
-
Counsel family members regarding their potential genetic risk.
Precision Medicine—using an individual’s genetic profile to guide clinical care (5)—shifts the paradigm from reactive treatment to proactive prevention. In the context of Malignant Hyperthermia, knowing the risk before the first incision is the most effective way to ensure patient safety.
References
1. Rosenberg H, Sambuughin N, Riazi S, Dirksen R. Malignant Hyperthermia Susceptibility. GeneReviews®.
2. Gonsalves SG, Dirksen RT, Sangkuhl K, et al. CPIC Guideline for the Use of Volatile Anesthetic Agents and Succinylcholine. Clin Pharmacol Ther.
3. Cong Z, Wan T, Wang J, et al. Epidemiological and clinical features of malignant hyperthermia. Clin Genet. 2024.
4. Groth CM, Acquisto NM. Genetic Testing for Malignant Hyperthermia Susceptibility. Genes (Basel). 2025.
5. Miller DT, Lee K, Abul-Husn NS, et al. ACMG SF v3.2 list for reporting secondary findings. Genet Med. 2023.
6. Riazi S, Kraeva N, Hopkins PM. Updated guide for the management of malignant hyperthermia. Can J Anaesth.
7. Merritt A, Booms P, Shaw MA, et al. Assessing pathogenicity of RYR1 variants. Br J Anaesth.
8. PharmGKB. RYR1 Gene Summary and CPIC Guideline Annotation.