Hemorrhoids are enlarged, bulging veins within and around the anal canal. The two groups of hemorrhoids are external and internal hemorrhoids which are differentiated by their location. The internal hemorrhoid problems can be classified as per the severity, ranging from grade 1 without prolapse to grade 4 in which hemorrhoid remains prolapsed outside of the anus. Although several treatment options are available, a number of patients prefer a minimally invasive approach. The combination of advances in the technology and the outstanding experience of the colorectal surgeons now offer a minimally invasive technique called “Transanal Hemorrhoidal Dearterialization” or THD as a novel treatment alternative. Compared to other surgical options, the superiority and advantages of THD include; less pain and fewer procedure-related complications as well as minimizing the chance of recurrence.
Minimally invasive treatment for hemorrhoids
The “transanal hemorrhoidal dearterialization” or THD is a minimally invasive technique to encounter the symptomatic hemorrhoids. During the procedure, a special designed anoscope armed with a Doppler transducer is used to identify the hemorrhoid arteries that supply the hemorrhoids. Once the hemorrhoid arteries are detected, a suture ligation is conducted in order to limit the blood flow to the hemorrhoid. In the case of redundant prolapse, the lifted suture (rectopexy) will allow the repositioning hemorrhoids back to the normal anatomical position. The ligation of hemorrhoid arteries will provide a significant reduction of the blood flow to the hemorrhoids, resulting in shrinkage of the hemorrhoids without the need for surgical removal.
The severity of hemorrhoids and THD
THD is recommended in patients who have had grade 3 internal hemorrhoids (defined as prolapsed internal hemorrhoids which do not go back inside the anus without the manual reduction) and grade 4 internal hemorrhoids (defined as prolapsed internal hemorrhoids with inability to be manually reduced). To achieve the best possible treatment outcomes, it is essential to seek the medical attention from the expert and highly experienced colorectal specialist.
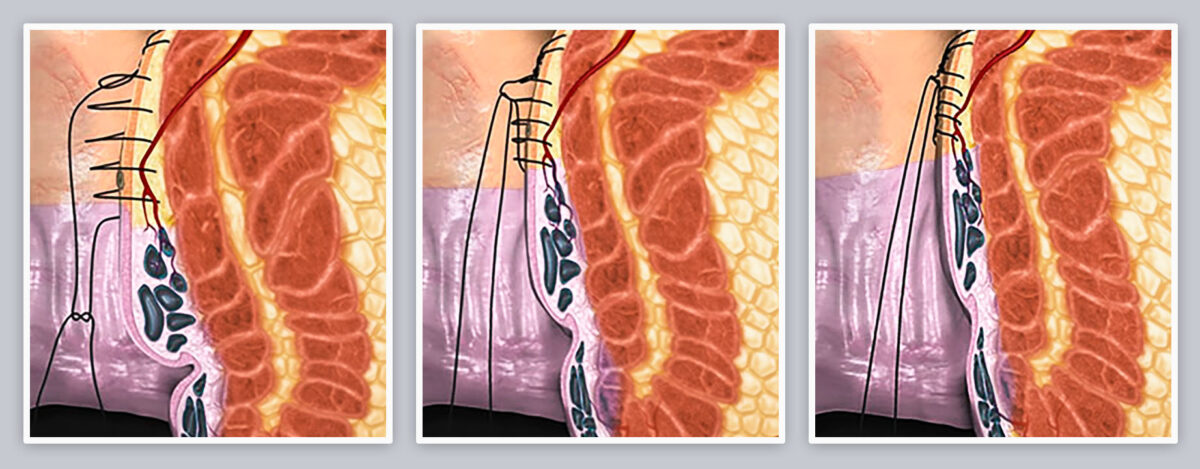
Steps during Transanal Hemorrhoidal Dearterialization (THD)
- Once the hemorrhoid arteries are detected, a suture ligation is conducted in order to limit the blood flow to the hemorrhoid.
- For redundant prolapse, the lifted suture (rectopexy) allows the hemorrhoids to be repositioned to the normal anatomical position.
Superior advantages of THD
- No incision or cut
- Minimal discomfort
- Less blood loss
- Rapid recovery and the hospitalization might not be required
- Maintained normal bowel movement
- Less procedure-related complications
Possible effects after treatment
Minor effects after THD might rarely develop, including
- Difficulty passing urine, often temporarily
- Bleeding
- Discomfort or pain
Lifestyle modifications to prevent recurrence
- Drink plenty of water at least 8-10 glasses/day to keep the soft stool.
- High-fiber diet including as fruits and vegetables.
- Avoid prolonged sitting in the toilet and excessive strain during the bowel movements.
- Frequently observe blood in the stool.
- Avoid heavy lifting or heavy weight-lifting exercise.
- Avoid processed foods and alcohol consumption.
The lack of awareness of having enlarged hemorrhoids can potentially lead to serious complications. In fact, the hemorrhoid issues can be effectively overcome using several treatment options based upon the symptoms and severity. Do not hesitate to get the medical attention for the appropriate advice and care provided by the expert specialists.