Monkeypox is worrying and interesting to many people. There are so many questions out there. The more we know, the better prepared we are to handle it.
Q: What is monkeypox?
A: Monkeypox is an infectious virus that causes mild symptoms. It belongs to the orthopoxvirus family, which is the same as the smallpox virus. It is often found in Central and West Africa. Although symptoms are not so severe and the risk of infection is low, it is commonly found in children. Thus, parents need to pay close attention.
Q: How does monkeypox spread?
A: Monkeypox can spread from:
- Animals to humans through direct contact with any animal that bites. Contact with bodily fluids, including blood, puss, and saliva from infected animal can introduce the virus into humans as well as eating uncooked infected meat.
- Humans to humans transmission occur from direct contact with droplets from coughing sneezing, rashes, pusses, and other infectious bodily fluids, which tend to come from sharing items.
Q: What are the symptoms of monkeypox?
A: Monkeypox has an incubation period of about 5 – 20 days. Symptoms can appear earlier if a person comes into contact with high virus load. However, with low amount of exposure, symptoms will appear about 3 weeks after exposure. Clear signs include fever, chills, body aches, back pain, eye pain, muscle aches, sore throat, and fatigue. Then, small red rashes or bumps begin to appear throughout the body 4 – 5 days later. These will turn into large vesicles with fluids inside. Some may burst. The degree of illness depends on each person and how much they have been exposed to the virus, but they tend to be non-life threatening.
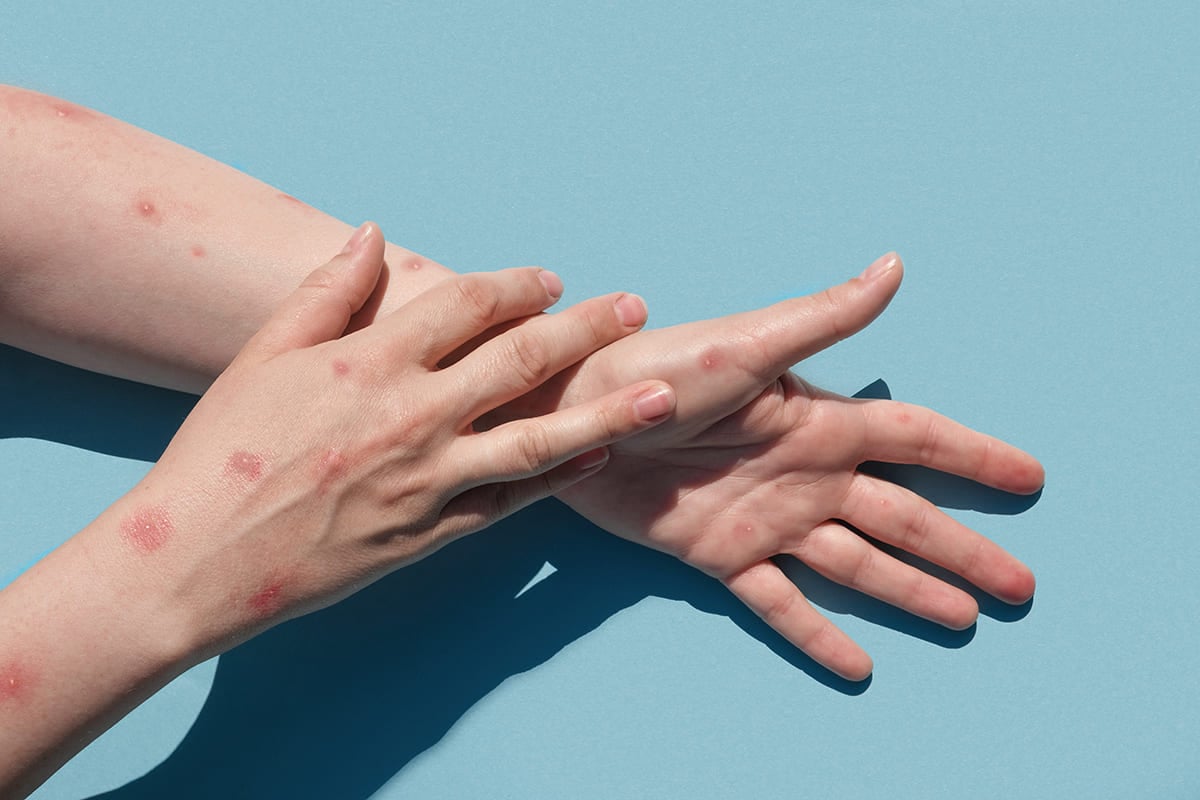
Q: How do doctors diagnose it?
A: Medical specialists will assess the symptoms, particularly fever with pustules are clear signs of monkeypox. Real-time PCR can be performed to identify the viral DNA within 24 – 48 hours. Then, DNA sequencing can be done to confirm, which takes additional 4 – 7 days.
Q: What should we do if we have monkeypox?
A: The affected person should be isolated immediately. Use separate bedroom, bathroom and personal items and do not come into contact with someone else. Most importantly, do not scratch, peel or pop the lesions since it may cause scarring that affects self-confidence.
Q: Will monkeypox go away by itself?
A: Monkeypox can go away by itself. It is not life-threatening and will take about 2 – 4 weeks to be cured. Some antiviral medications can combat smallpox and monkeypox.
Q: How can we prevent monkeypox infection?
A: Preventive measures include wearing a mask, frequent handwashing, avoid touching your face, eyes, nose and mouth, avoid getting scratched or bitten by animals, do not share use of personal items, and keep away from infected person.
Q: Which animals that can be reservoir for monkeypox?
A: All animals that can bite, not just monkeys, can carry monkeypox. Be particularly careful of rodents, squirrels, and rabbits.
Q: Is there a vaccine for monkeypox?
A: Vaccines against smallpox can also prevent monkeypox. Older adults who have had smallpox vaccine will be immunized against monkeypox. However, people who were born after 1980 may not have received smallpox vaccine. Currently, a smallpox live-attenuated virus vaccine manufactured by a Danish company is available, It is made from a Modified Vaccinia Ankara Bavarian Nordic, a closely related virus to smallpox. However, the efficacy and side effects are still unclear. Since monkeypox is still not considered a pandemic, the vaccine currently not available in Thailand.
Q: Can previous vaccine inoculation prevent monkeypox?
A: People who have had smallpox vaccine inoculation in the past will help prevent monkeypox. However, because smallpox has been eradicated by 1974, Thailand began stopping inoculation around that time. If you are wondering about whether you had vaccination or not, look for a flat or slightly dented scar on your left arm as well as your birth year. People who were born after 1980 definitely will not have had smallpox vaccination. People who were born between 1974 and 1980 may or may not have been inoculated. Please check with a healthcare specialist to confirm.