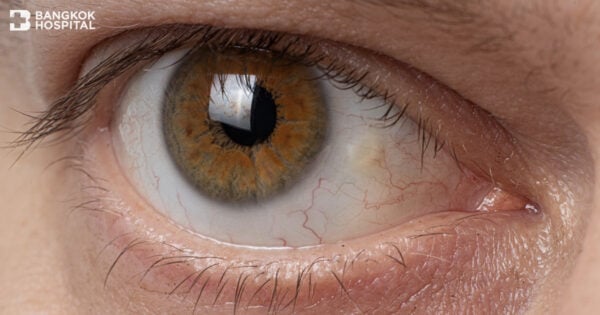
Pinguecula and pterygium are the common degenerations of the conjunctiva. A pinguecula is characterized by a yellowish raised growth on the conjunctiva typically at the nasal or temporal conjunctiva near the edge of cornea. Pterygium is the triangular shape of vascularized conjunctival tissue on the cornea and it invades the cornea (known as fibrovascular invasion of the cornea). Pterygium may start as a pinguecula that can remain small or grow large enough to cover some parts of the cornea. The body of a pterygium usually appears red with noticeable blood vessels. Redness depends on the growth of abnormal blood vessels. If it is left untreated, pterygium sometimes advances towards the center of the eye, affecting vision. They are not tumor. Generally, pinguecula and pterygium form in the corner of the eye near the nose. However, they may develop in the temporal of the eye and often both eyes are involved.
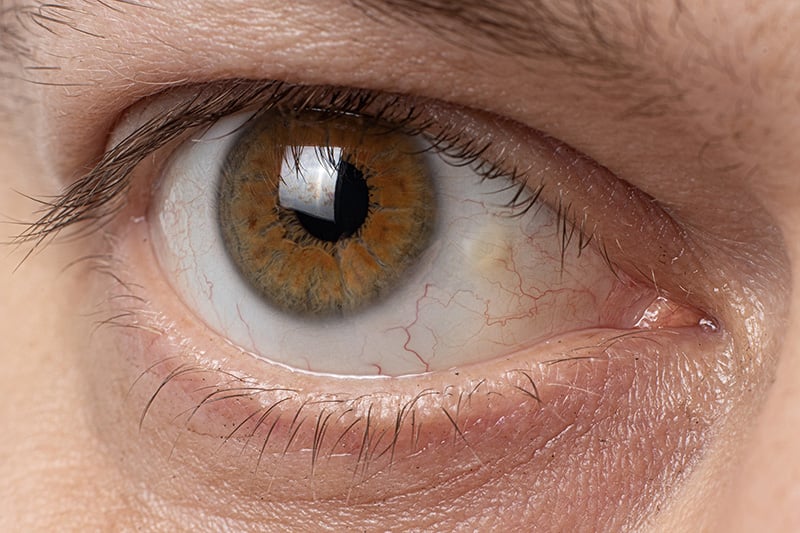
(Pinguecula)
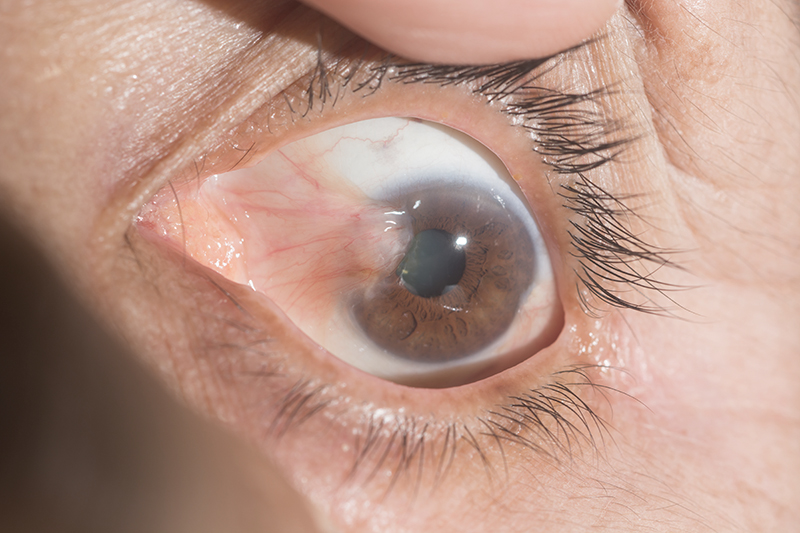
(Pterygium)
Causes of pinguecula and pterygium
Chronic exposure to sun and ultraviolet (UV) radiation is thought to be the most common cause for the development of pinguecula and pterygium although it typically takes months or years. Since UV light is a causal factor, pinguecula and pterygium are frequently found in people who live in warm and dry climate (tropical area) or expose to the sun during their work or activities. In fact, certain lamps or light bulbs can emit UV ray which becomes another source of UV radiation. In addition, exposure to wind, sand or dust for a long period of time are contributing factors to cause inflammation of pinguecula and pterygium.
Signs and symptoms of pinguecula and pterygium
Most patients who develop pinguecula or early pterygium are asymptomatic, whereas some experience only mild symptoms, presenting with an abnormal growth of tissue on the conjunctiva. If the condition progresses with inflammation, patients often exhibit relevant symptoms, including pain, discomfort or irritation in the affected eye, eye itchiness or redness and watery eye. Some patients may sometimes have a gritty or burning feeling in the eye. Besides UV light, exposure to wind, dust, sand or smoke can aggravate the symptoms.
In patients who have pterygium, blurry vision and astigmatism may develop if the cornea is distorted and corneal curvature is altered due to the extension of the pterygium onto the cornea. If the condition persists, the pterygium grows across to central cornea, resulting in marked decrease vision. Pinguecula and pterygium can be present in one or both eyes. Although these conjunctival degenerative conditions can strike anyone, adults and the elderly are more likely to develop pinguecula and pterygium due to long-term exposure to trigger factors.
Treatment of pinguecula and pterygium
Among different treatment options, ranging from lifestyle modification to eye surgery, appropriate treatment for pinguecula and pterygium depends upon disease severity while taking each patient’s condition into consideration. If the size of pinguecula or pterygium is considerably small without eye irritation and visual distortion, treatment mainly involves lifestyle modifications to prevent disease progression. These include wearing certified sunglasses and brimmed hats or other sun and wind protective equipment while outdoors. Some prescription glasses have certain lenses capable of protecting the eyes from ultraviolet rays.
For patients with eye discomfort, artificial tears, gels or ointments and other eye drops, e.g. topical steroid drops might be prescribed to reduce the inflammation and relieve relevant symptoms caused by inflammation. Nonetheless, if pterygium grows and invades into the cornea, causing chronic inflammation,irritation symptoms and vision problems such as astigmatism and blurry vision, the ophthalmologist might potentially consider eye surgery to remove the abnormal tissue from the sclera and cornea of the eye. Today’s technique, minimally invasive pterygium surgery with grafting offers a significantly higher success rate than conventional surgery.
Pterygium poses high recurrence rates after surgical removal, particularly in young patients with continual exposure to UV radiation. Several predisposing factors are associated with pterygium recurrences. To minimize the chance of recurrent pterygium, pterygium excision combined with graft – a standard technique shows a promising outcome.
After the removal of the pterygium, a graft is attached to bare area to prevent recurrence. Tissue grafts can be derived from either conjunctival tissue from superior part of the patient’s eye (conjunctival autograft) or preserved amniotic membrane graft (from The Thai Red Cross Society) After tissue grafts are placed in the region of scleral exposure, either tiny sutures or fibrin glue, a biological tissue adhesive (tissue sealant) are used to secure the conjunctiva tissue graft in its place.
During the surgery, adjuvant therapies such as mitomycin-C application might be given to reduce postoperative conjunctival inflammation, leading to less chance of pterygium recurrences. Pterygium eye surgery is performed under local anesthesia on an outpatient basis and it normally takes 30-40 minutes. Using minimally invasive technique, patients achieve faster recover with a quick return to their daily lives.
Prevention of pinguecula and pterygium
- Protect the eye from ultraviolet radiation by wearing brimmed hats and sunglasses with lenses that can effectively block ultraviolet light while outdoors. Regardless of sunlight, sunglasses need to be worn in order to prevent wind, dust and sand.
- Avoid warm or dry climate or smoky and windy environment that triggers inflammation and exacerbates symptoms, e.g. dry eye and eye irritation.
- Frequently notice a change in the appearance of the eye. If pinguecula or pterygium is existing, regularly observe its size, color and shape. If any change is noticed, seek medical assistance immediately.
- To minimize the chance of recurrence after pterygium eye surgery, it is still crucial to refrain from UV exposure.