Spondylosis refers to degenerative changes in the spine such as bone spurs and degenerating intervertebral discs between the vertebrae.
Spondylosis changes in the spine are frequently referred to as osteoarthritis. It is a general term for age-related wear and tear affecting the spinal disks. Apart from advancing age and genetic effects, lifestyle and previous spine injuries are the major risk factors of developing spondylosis. Cervical spondylosis is the most common type of progressive spondylosis that affects the neck. Other types of spondylosis may develop in different parts of the spine such as thoracic spondylosis (affecting the middle of the spine), lumbar spondylosis (affecting the lower back) and multilevel spondylosis which affects more than one part of the spine. As the disks dehydrate and shrink, signs of spondylosis develop, including stiffness and pain that get worse following certain movements or long periods without moving, while sitting for a long time. To diagnose spondylosis, physical examinations involve checking the range of motion and testing reflexes and muscle strength to find out pressure on spinal nerves or spinal cord as well as nerve function tests. In addition, imaging tests to investigate spondylosis are X-ray, CT and MRI. Selected treatments are primarily determined by presenting symptoms, disease severity and individual conditions of the patients. A wide range of treatment options include non-surgical approach and surgery. Non-surgical treatments include oral medications (nonsteroidal anti-inflammatory drugs, corticosteroids, muscle relaxants, some anti-seizure medications and anti-depressants), injections and rehabilitation e.g. ultrasound treatment and electrical stimulation. Nevertheless, if symptoms progress without proper responses to previous non-operative treatments, spinal cord or nerve roots become severely compressed, resulting in serious complications such as spondylolisthesis, a slipping of spine. In such a case, spine surgery might be highly considered.
Spine surgery is traditionally done as open surgery with a long incision to allow the surgeon to visualize and access the surgical field. In recent years, technological advances have allowed spine conditions including spondylosis to be treated with a minimally invasive spine surgery (MISS).
Instead of having a long incision that is required for open surgery, minimally invasive spine surgery is performed through smaller incisions. This less invasive technique avoids significant damages to surrounding muscles and nerves. Typically, it results in less pain and fewer postoperative complications, leading to a faster recovery. More importantly, minimally invasive technique largely enhances the accuracy and precision on screw fixation, resulting in minimized chances of having complications caused by misplaced screws e.g. severe pain that radiates to the legs and permanent disability.
There are various minimally invasive spine techniques. The common goal among all of them is that they use smaller incisions and cause less muscle and nerve damages. Minimally invasive techniques can be used for common procedures such as lumbar decompression and spinal fusion. Decompression relieves pressure on spinal nerves by removing portions of bone or a herniated disk. While spinal fusion corrects problems with the small bones of the spine. The basic idea is to fuse together the painful vertebrae so that they heal into a single solid bone.
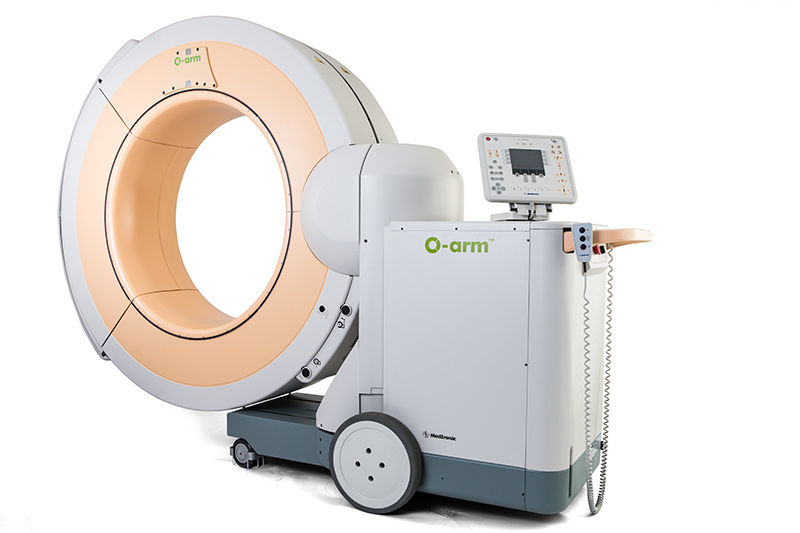
Improving surgical outcomes with O-arm, surgical imaging system that enhances accuracy and safety while operating
The O-arm Surgical Imaging System is a surgical imaging platform designed for minimally invasive spine surgery. Due to its advancements in imaging, it provides real-time, intra-operative images of a patient’s anatomy with high quality and a large field-of-view in both two and three dimensions.
The O-arm system has been designed to optimally support patient’s safety and surgical workflow. Its unique gantry provides vital lateral patient access, essential for optimal patient positioning and allowing high degree of flexibility during operation. The O-arm System seamlessly integrates with Stealth Station, a navigation system to reduce X-ray exposure. The use of the O-arm and Stealth Station dramatically increases safety the patients. Surgical Navigation provides the surgeon with real-time information about the patient’s anatomy while reducing the X-ray exposure to patient, surgeon and staff. For spinal surgery, a wide range of dedicated navigated instruments and referencing frame options allow to optimize the use of navigation in each part of the spine. As a result, minimally invasive spine surgery can be performed with improved accuracy, precision and safety.
In the conventional approach, intra-operative C-Arm fluoroscopy is typically used to provide 2D images of patient’s anatomy. Nonetheless, the image quality might not be sufficient to visualize and evaluate the surgical accuracy, leading to misplaced screws that eventually cause other serious complications. Superior benefits of the O-arm and navigation system include:
- The O-arm is fully mobile and it can be easily brought for use in concurrent cases and imaging on demand at any time during a procedure.
- Through robotic positioning, the O-arm remembers the best surgical views. Programmable memory stores the exact position of the gantry and detector. The exact image positions can be recalled at the touch of a button any time during surgery, eliminating time-consuming repositioning and additional X-ray exposure.
- The O-arm and Stealth Navigation help to verify the exact location of the screws placed to fix the affected spine. The system ensures safety that surrounding nerves and muscles will not be damaged during surgery. In addition, high quality 3D images obtained from the software precisely guide the surgeon to correct the problems in the affected areas.

Although spine surgery might sound frightening for some people, advanced technology in minimally invasive spine surgery supported by the O-arm and Stealth Navigation System largely brings satisfied outcomes. Due to smaller incisions, patients often experience les pain and faster recovery time. Additionally, navigation system greatly enhances safety and reduces postoperative complications e.g. fewer blood loss, lowered rates of infection and less damage to surrounding nerves and muscles. Patients can rest assured that their treatment outcomes will be safe, accurate and effective with close-to-zero chances of postoperative complications.










