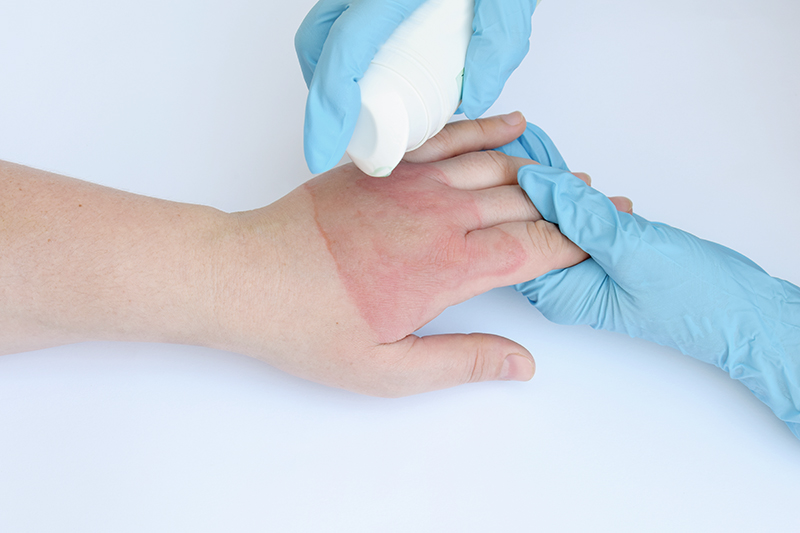
Burns are characterized by tissue skin damages that mainly result from dry heat e.g. flames and heated clothing iron or moist heat e.g. boiled water and hot coffee. Other possible causes of burns include an exposure to chemical substances, electrical contact and overexposure to the sun or other radiation. Burns can be minor medical problems or life-threatening emergencies, depending on the severity of damage to the skin.
Burns are one of the most common wound problems. Burn symptoms vary depending on how deep and how large the skin damage is. If burns are large and affecting deeper layer of skin, it can cause severe pain, prolonged treatment with higher hospital expenditure, disfigurement and disability. Moreover, if burns are severe, receiving intensive treatment in the hospital is vitally required since fatal complications might develop, leading to an increased chance of death.
Severity of burns
Severity of burn injury is determined by the depth of skin damage (degrees of burns) and the size of the wound. Burns are divided into 4 categories:
- First-degree burn. This type is minor burn, affecting only the outer layer of the skin (epidermis). It might cause mild redness and pain. It is usually self-limiting. First-degree burn usually needs a week healing time, without scarring. The example of this type of burn is overexposure to the sun (sunburns)
- Superficial second-degree burn. This type of burn affects both the epidermis and the superficial layer of the dermis which is the second layer of skin. Blisters may develop and pain can be severe. It may cause white or splotchy skin. If treated appropriately, burns can be cured within 2-3 weeks and scar rarely occurs.
- Deep second-degree burn. This type of burn affects the epidermis and the deeper layer of the dermis, making it more difficult to treat. It usually requires longer healing time and it can cause scarring.
- Third-degree burn. This burn damages the entire layers of the skin and reaches to the fat layer beneath the skin. Third-degree burn can destroy nerves, causing numbness and less pain. Burned areas may turn to be white. The skin may look leathery or cover with necrotic tissue. Third-degree burn has a high risk of infection. Treatments are complicated. It is usually treated with skin grafts by surgical removal the injured skin and replacing it with healthy skin from an uninjured area of the body (skin grafting). However, if it is a small burn, it can be self-limiting and scarring after burns usually develops.
The size of burns can be estimated as the percentage of body surface area burned by using the rule of palm. The palm of the patient who is burned is about 1% of the body. Another method for adult is called the rule of nines. In this method, the body is divided into sections of 9%, each arm is equal to 9% of body surface area and each leg is equal to 18% of body surface area. The treatment of burns depends on the severity and location of skin damage. Deep or widespread burns often need immediate medical attention. Some patients with severe burns need treatment at specialized burn centers and several months for follow-up care.
Treatment of burns
If burns happen, appropriate first aid care must be timely applied as follows:
- Wash your hands and rinse the wounds with clean water. For dirty wounds, wash around the wound with soap and water.
- If applicable, rinse the wound or put the wound in room temperatue water as soon as possible. Continue wound compression at least 5 minutes, but not longer than 20 minutes. Do not use cold water or ice since it can deepen the depth of the tissue damages.
- Cover the wound by applying a bandage, rolled gauze or gauze in place with tape and seek immediate medical attention. Do not apply toothpaste or other lotions or ointments to the wounds since it might increase chances of skin infection.
Before treatment, the doctor starts conducting wound assessment to determine the severity, location and size of burns. Treatments usually involve wound dressings, medication and may surgery, if needed. The goals of treatment are to control pain, remove necrotic tissue, prevent complications e.g. infection, reduce scarring and restore function.
At first, wounds need to be properly cleaned. If necrotic or dead tissue is found, it must be removed. Antibiotic creams or ointments might be applied to the affected areas. Wound can be closed by advanced wound closure devices. If the wounds are large or occurring in the major part of the body e.g. face, hands and perineum, patients might need to be hospitalized.
Wound dressing is conducted with continuous wound assessment. If necrosis develops, dead tissue needs to be regularly removed everyday or every 1-4 days, depending upon individual conditions. Antibiotic and pain killer medicines might be prescribed if necessary. If the skin damages are not deep, the wounds are usually self-limiting with complete cure in 1-3 weeks. However, for more severe wounds with higher degree burns, skin grafting might be required. A skin graft is a surgical procedure in which sections of patient’s own healthy skin are used to cover the deep burns. Donor site wounds take on average 2-3 weeks to automatically heal. Skin obtained from other people is disallowed since a skin transplant between two people can cause a rejection process where the immune system of the recipient or host attacks the foreign donor tissue.
Due to the advancements in medical technology, wound care for burns has been drastically improved. Advanced wound dressing and proper wound care given by highly expert specialists and multidisciplinary team substantially help to heal the wound faster alleviate physical pain and emotional distress caused by burns. If burns inevitably occur, immediate medical assistance must be sought in order to receive timely and appropriate treatments.